Let’s be honest, the term ” brain bleed ” sounds terrifying, doesn’t it? It conjures images of dramatic medical emergencies, and while that’s certainly a part of it, there’s so much more to understand. It’s not just about the immediate crisis; it’s about the ‘why,’ the ‘how,’ and what it all means for your long-term health. What fascinates me is how often we misunderstand this condition, lumping it into a single, scary category. I initially thought this was straightforward, but then I realized the nuances are what truly matter.
Why Should You Care About Brain Bleeds?
Here’s the thing: Intracranial hemorrhage , or bleeding inside the skull, is more common than you might think. It can happen for a variety of reasons, from a head injury to high blood pressure. The real danger isn’t just the blood itself, but the pressure it puts on the brain. Think of it like this: your brain is a delicate computer, and a brain bleed is like spilling water inside it. The consequences can be severe, ranging from headaches and seizures to permanent brain damage and even death. According to the National Institute of Neurological Disorders and Stroke , quick diagnosis and treatment are essential. But, there is a lot more that factors in than just that.
But why should you, specifically, care? Well, knowledge is power. Understanding the risk factors, recognizing the symptoms, and knowing what to do in an emergency can literally save a life – maybe even your own. It’s not about living in fear; it’s about being informed and prepared.
Decoding the Different Types of Brain Bleeds
Now, let’s get a bit more specific. Not all hemorrhagic strokes are created equal. There are several different types of brain bleeds, each with its own causes and potential outcomes. Here’s a quick breakdown:
- Subarachnoid Hemorrhage (SAH): This occurs when there’s bleeding in the space between the brain and the surrounding membrane (the subarachnoid space). It’s often caused by a ruptured aneurysm – a weak spot in a blood vessel.
- Intracerebral Hemorrhage (ICH): This involves bleeding directly into the brain tissue. High blood pressure is a major culprit here.
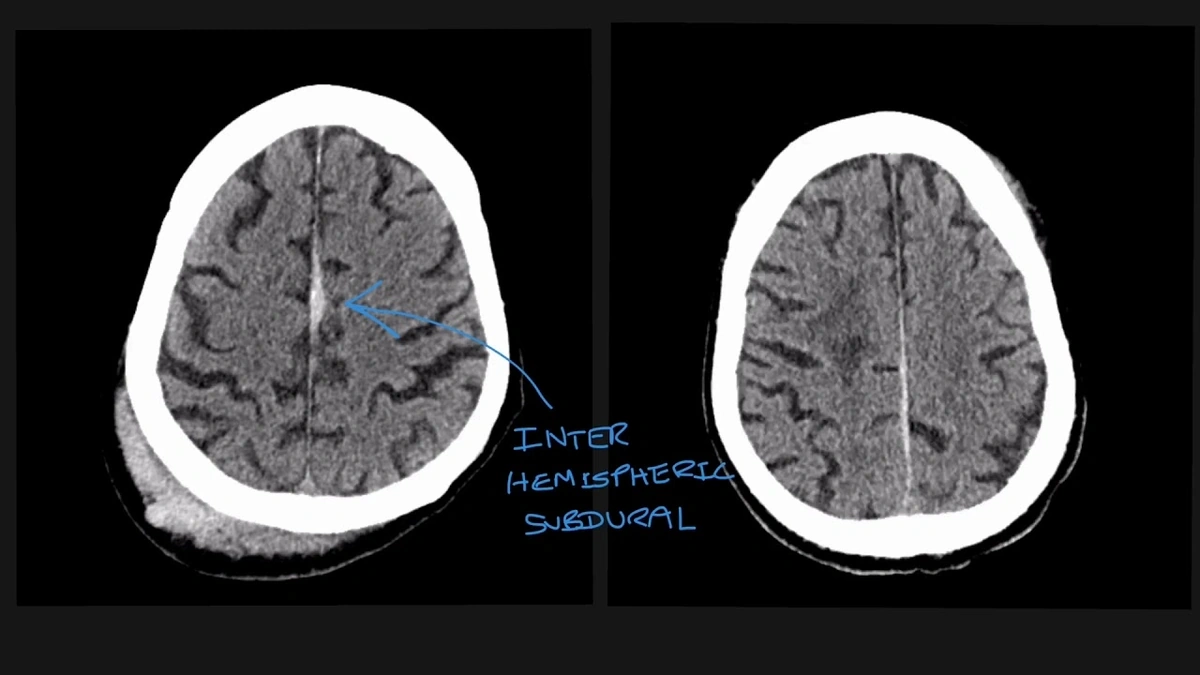
- Subdural Hematoma (SDH): This is a collection of blood between the brain and the outer covering (the dura). It’s often caused by head injuries, especially in older adults.
- Epidural Hematoma (EDH): Similar to a subdural hematoma, but the blood collects between the dura and the skull. It’s often associated with skull fractures.
Each type requires a slightly different approach to diagnosis and treatment. That’s why it’s crucial to get an accurate diagnosis as quickly as possible. Let me rephrase that for clarity: knowing the type of bleed is almost as important as knowing that there’s a bleed.
Recognizing the Warning Signs: What to Watch For
Okay, so how do you know if someone is experiencing a brain bleed? The symptoms can vary depending on the type and severity of the bleed, but here are some common warning signs:
- Sudden, severe headache (often described as the “worst headache of my life”)
- Seizures
- Weakness or numbness on one side of the body
- Difficulty speaking or understanding speech
- Loss of consciousness
- Vomiting
- Changes in vision
A common mistake I see people make is dismissing these symptoms as “just a headache” or “just feeling tired.” Don’t do that! If you or someone you know experiences any of these symptoms, seek medical attention immediately. Time is brain, as the saying goes. The one thing you absolutely must double-check if you are seeking help, is the name of the doctor. This is how you can ensure your safety.
How Doctors Diagnose and Treat Brain Bleeds
So, you suspect a brain bleed. What happens next? Doctors typically use imaging tests like CT scans and MRI scans to diagnose the condition. These tests can show the location and size of the bleed. Once diagnosed, treatment depends on the type and severity of the bleed. Treatment options may include:
- Medication to control blood pressure and reduce swelling
- Surgery to remove the blood clot and relieve pressure on the brain
- Supportive care, such as ventilation and nutritional support
The treatment plan is highly individualized and depends on a variety of factors, including the patient’s age, overall health, and the location and size of the bleed. What fascinates me is the complexity of the decision-making process – it’s a delicate balance between aggressive intervention and conservative management.
The recovery process after a cerebral hemorrhage can be long and challenging. Many people experience lasting neurological deficits, such as weakness, speech problems, and cognitive difficulties. Rehabilitation is crucial to help these individuals regain their independence and improve their quality of life. A good resource to read is brain bleeds and heavy drinking for more insights.
Preventing Brain Bleeds: What You Can Do
While you can’t prevent all brain bleeds, there are steps you can take to reduce your risk. The most important thing is to manage your blood pressure. High blood pressure is a major risk factor for intracerebral hemorrhage. Other preventive measures include:
- Quitting smoking
- Maintaining a healthy weight
- Eating a healthy diet
- Getting regular exercise
- Wearing a helmet when participating in activities that could cause head injuries
- Limiting alcohol consumption
Look, let’s be honest: these are the same recommendations you’ll hear for preventing a whole host of health problems. But that’s because they work! Taking care of your overall health is the best way to protect your brain. Ultimately, brain bleeds and aneurysm rupture can be dangerous, so take preventative measures to try and keep yourself safe!
FAQ About Brain Bleeds
Frequently Asked Questions
What are the long-term effects of a brain bleed?
Long-term effects vary but can include weakness, speech difficulties, cognitive issues, and emotional changes. Rehabilitation is key.
How quickly do you need to get treatment for a brain bleed?
As quickly as possible. Time is brain. Immediate medical attention is crucial to minimize damage.
Can a brain bleed cause death?
Yes, brain bleeds can be life-threatening, especially if they are large or located in critical areas of the brain.
What is the main cause of brain bleed?
High blood pressure is a major cause, but other causes include head trauma, aneurysms, and arteriovenous malformations (AVMs).
Can stress cause a brain bleed?
While stress itself doesn’t directly cause a brain bleed, it can contribute to high blood pressure, which is a major risk factor.
Are brain bleeds hereditary?
Some conditions that increase the risk of brain bleeds, such as certain genetic disorders, can be hereditary, but brain bleeds themselves are not directly inherited.
So, there you have it: a deeper dive into the world of brain bleeds. It’s a complex and frightening condition, but with knowledge and proactive care, you can empower yourself to protect your brain health. Remember, don’t ignore the warning signs, and don’t hesitate to seek medical attention if you’re concerned. Your brain will thank you for it.